Exploring the Latest Advances in Atrial Fibrillation Treatment
Lorem ipsum dolor sit amet, consectetur adipiscing elit.
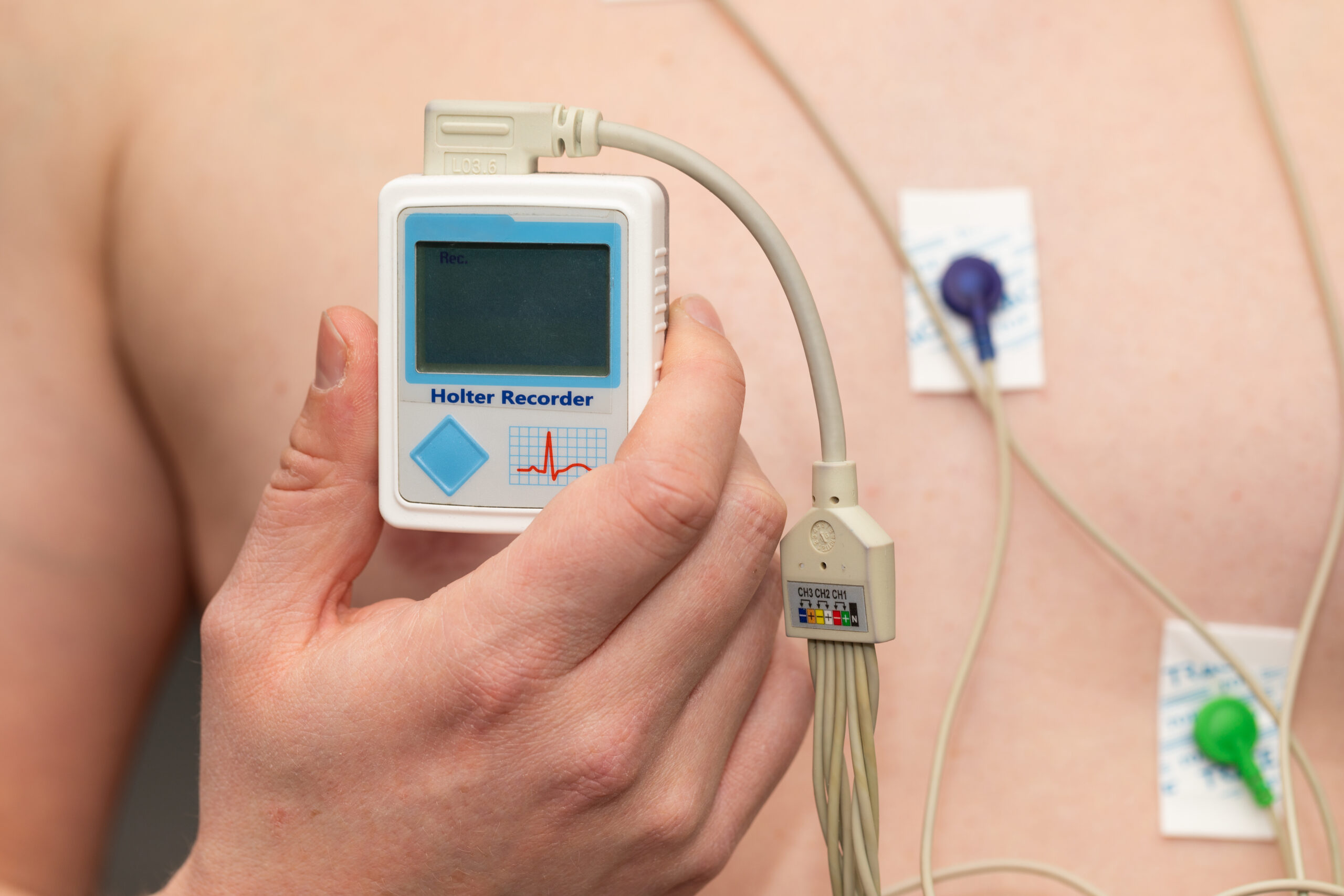
Exploring the Latest Advances in Atrial Fibrillation Treatment: A Comprehensive Guide for Patients and Caregivers
Seeking treatment from our Atlanta heart doctors can be a game-changer for your health and quality of life. AFib is a common heart rhythm disorder that, if left untreated, can lead to serious complications. Let’s explore how our cardiology team can help you manage this condition effectively.
Atrial fibrillation occurs when the upper chambers of your heart beat irregularly and often rapidly. You might experience symptoms like heart palpitations, shortness of breath, fatigue, or dizziness. However, some people with AFib don’t notice any symptoms at all, which is why regular check-ups with a cardiologist are crucial.
You’ll receive a comprehensive evaluation when you visit our Atlanta heart clinic for AFib treatment. This typically includes a detailed medical history, physical examination, and diagnostic tests such as an electrocardiogram (ECG) or echocardiogram. These tests help our doctors understand the severity of your AFib and any underlying heart conditions.
Treatment for AFib is highly individualized, and our Atlanta cardiologists will work with you to develop a plan that fits your specific needs. The main goals of treatment are to control your heart rate, restore a normal rhythm if possible, and prevent blood clots that can lead to stroke.
For many patients, medication is a key component of AFib management. Our doctors might prescribe drugs to control your heart rate or rhythm. Anticoagulants, often called blood thinners, are also commonly used to reduce the risk of stroke in AFib patients.
In some cases, a procedure called cardioversion might be recommended. This involves using electrical shocks or medication to reset your heart’s rhythm. It’s a controlled, scheduled procedure that our experienced cardiologists perform regularly.
Our Atlanta heart doctors might suggest catheter ablation for patients who don’t respond well to medication or cardioversion. This minimally invasive procedure targets the areas of your heart, causing an irregular rhythm. While it’s not a cure for everyone, many patients experience significant improvement in their symptoms and quality of life after ablation.
Lifestyle modifications play a crucial role in managing AFib. Our cardiology team will guide you on heart-healthy habits such as maintaining a balanced diet, staying physically active, managing stress, and avoiding triggers like excessive alcohol or caffeine consumption.
Regular follow-up appointments are essential in AFib treatment. These visits allow our doctors to monitor your condition, adjust your treatment as needed, and address any concerns you might have. We’re committed to partnering with you for the long term to keep your AFib under control.
While AFib is a chronic condition, it doesn’t have to control your life. With proper treatment and management under the care of our Atlanta heart specialists, many people with AFib lead full, active lives.
Early intervention can significantly improve AFib treatment outcomes. If you’re experiencing symptoms or have concerns about your heart rhythm, don’t hesitate to contact our Atlanta cardiology clinic. Our team of experienced heart doctors is here to provide expert care, advanced treatment options, and ongoing support in managing atrial fibrillation.
By choosing our Atlanta heart doctors for your AFib treatment, you’re taking a proactive step towards better heart health and a more vibrant life. Let us help you regain control of your heart rhythm and reduce your risk of AFib-related complications.
Read about AFib causes, treatment, and how CVG provides comprehensive cardiac care.
What is AFib and How is It Treated?
Understanding Atrial Fibrillation
Atrial fibrillation (AFib) is a common cardiac arrhythmia that affects millions of people worldwide. It occurs when the heart’s electrical signals become disorganized, leading to an irregular heartbeat. This can cause the heart’s atria (upper chambers) to quiver instead of contracting normally, leading to poor blood flow to the rest of the body.
The symptoms of AFib can range from mild to severe, and some people may not experience any symptoms at all. Common symptoms of AFib include palpitations or the sensation of a racing or fluttering heartbeat, shortness of breath, dizziness or lightheadedness, chest pain or discomfort, and fatigue or weakness. Sometimes, AFib can lead to more serious complications such as stroke or heart failure.
There are several known risk factors for AFib, including high blood pressure, coronary artery disease, heart valve problems, obesity, diabetes, sleep apnea, and excessive alcohol or caffeine consumption. Other factors such as age, genetics, and certain medical conditions such as thyroid disease or lung disease can also increase the risk of developing AFib.
The treatment of AFib typically involves managing the underlying causes and reducing symptoms. This can include lifestyle changes such as reducing alcohol and caffeine consumption, quitting smoking, and maintaining a healthy weight. Doctors may prescribe medications such as blood thinners, heart rate control medications, and rhythm control medications to manage the condition.
Sometimes, electrical cardioversion may be recommended to restore a normal heart rhythm. This procedure uses an electrical shock to reset the heart’s electrical activity, allowing it to return to a normal rhythm. Electrical cardioversion has been an effective treatment for AFib, with a high success rate in restoring normal heart rhythm.
Conventional Atrial Fibrillatio Treatment Options
There are several conventional treatment options available for atrial fibrillation (AFib), depending on the severity and frequency of symptoms. These treatments include:
Medications:
Several medications are available that can help regulate the heart rhythm and reduce the risk of blood clots. Commonly used medications include beta-blockers, calcium channel blockers, and anti-arrhythmic drugs.
Cardioversion:
This procedure uses electrical shock or medication to restore the heart’s rhythm. There are two types of cardioversion: electrical cardioversion and pharmacologic cardioversion.
Catheter Ablation:
This is a minimally invasive procedure that uses radiofrequency energy or cryotherapy to destroy the small areas of the heart that are causing an irregular heartbeat.
Surgery:
In some cases, surgery may be necessary to treat AFib. One common surgery is the maze procedure, which creates scar tissue in the heart to redirect the electrical signals and restore normal rhythm.
Lifestyle Changes:
Making lifestyle changes such as quitting smoking, limiting alcohol and caffeine consumption, and managing stress can help reduce the risk of AFib and improve symptoms.
The individual’s specific condition and medical history will determine their treatment, which their healthcare provider will determine.
Besides the conventional treatment options mentioned above, healthcare providers may also recommend other strategies to manage atrial fibrillation (AFib) and its associated symptoms. These strategies may include:
Anticoagulation Therapy:
This therapy involves taking blood-thinning medications such as warfarin or newer oral anticoagulants to reduce the risk of blood clots and stroke in patients with AFib.
Rate Control:
This approach focuses on slowing the heart rate rather than restoring a normal rhythm. Medications such as beta-blockers or calcium channel blockers can achieve this.
Lifestyle Modifications:
In addition to the lifestyle changes mentioned in the previous section, other modifications, such as maintaining a healthy weight and engaging in regular exercise, may be recommended to manage AFib.
Holter Monitoring:
This portable device records the heart’s electrical activity over time, allowing healthcare providers to monitor and analyze abnormal rhythms.
It’s important to note that the treatment will depend on several factors, including the severity and frequency of symptoms, the patient’s medical history, and overall health. Patients with AFib should work closely with their healthcare providers to determine the best course of treatment for their individual needs.
Latest Advances in Atrial Fibrillation Treatment
There have been several recent advances in the treatment of atrial fibrillation (AFib), including:
New Medications:
Several new drugs have been developed to treat AFib, including novel anticoagulants that are more effective than traditional blood thinners and have fewer side effects. There are also new antiarrhythmic drugs that can regulate heart rhythm with fewer adverse effects.
Improved Catheter Ablation Techniques:
Catheter ablation has become a popular treatment for AFib in recent years, and new advances in this procedure have made it even more effective. One such technique is cryoablation, which uses extreme cold to freeze the areas of the heart that are causing irregular heartbeat.
Left Atrial Appendage Closure Devices:
The left atrial appendage is a small pouch in the heart where blood can pool and form clots in people with AFib. Left atrial appendage closure devices can be implanted to seal off this area and reduce the risk of stroke.
Wearable Technology:
Advances in wearable technology make monitoring heart rhythms continuously and remotely possible. This can be useful for people with AFib, as it allows their healthcare providers to detect and treat irregular heartbeats before they cause symptoms or complications.
Artificial Intelligence:
Artificial intelligence (AI) is being used to develop new tools for diagnosing and treating AFib. For example, AI algorithms can analyze electrocardiogram (ECG) data to detect irregular heartbeats and predict the likelihood of developing AFib in the future.
Overall, these advances in AFib treatment are promising and offer new options for people with this condition. Discussing these options with a healthcare provider to determine the best course of treatment for each case is important.
Factors to Consider When Choosing an Atrial Fibrillation Treatment
When choosing a treatment for atrial fibrillation (AFib), consider the following:
The Severity of Symptoms:
The severity and frequency of AFib symptoms will play a significant role in the type of treatment. For example, someone with mild symptoms may benefit from lifestyle changes or medication, while someone with more severe symptoms may require more aggressive treatment options.
Underlying Health Conditions:
The presence of other health conditions, such as high blood pressure, heart disease, or diabetes, may impact the treatment for AFib.
Risk of Stroke:
AFib can increase the risk of stroke, so the individual’s risk factors, such as age, history of stroke, or presence of other medical conditions, will need to be considered when choosing a treatment.
Side Effects:
All medications and procedures have potential side effects, so it is important to weigh the potential benefits of treatment against the possible risks and side effects.
Patient Preference:
The individual’s preferences, values, and lifestyle may also influence the treatment. For example, someone who prefers a more natural approach may focus on lifestyle changes, while someone who wants a more aggressive approach may opt for surgery or catheter ablation.
Cost:
The cost of treatment can also be a factor, as some treatments may be more expensive than others.
Ultimately, AFib treatment should be discussed with a healthcare provider, who can provide personalized recommendations based on the individual’s unique medical history and circumstances.
The Role of Patients and Caregivers in Atrial Fibrillation Treatment
Patients and caregivers play a crucial role in the treatment of atrial fibrillation (AFib). Here are some of the ways they can contribute:
Communication:
Effective communication with healthcare providers is essential for managing AFib. Patients and caregivers should ask questions and provide information about symptoms, medication side effects, and other concerns. Caregivers can also help keep track of medications, appointments, and test results.
Adherence to Treatment:
Patients must take medications as prescribed and follow other treatment recommendations, such as lifestyle changes. Caregivers can help by reminding patients to take their medications, assisting with lifestyle changes, and providing emotional support.
Monitoring:
Patients and caregivers can monitor symptoms and side effects of treatment and report any changes to the healthcare provider. They can also monitor blood pressure, heart rate, and other vital signs as directed by the healthcare provider.
Lifestyle Changes:
Lifestyle changes such as maintaining a healthy diet, exercising regularly, and avoiding alcohol and smoking can help manage AFib. Patients and caregivers can collaborate to develop and implement a plan for these changes.
Emotional Support:
AFib can be challenging to manage, causing emotional and psychological distress to the patient. The caregiver can help alleviate this by providing emotional support, such as listening, encouraging, and offering practical help.
Overall, patients and caregivers in AFib treatment should collaborate with healthcare providers, actively manage the condition, and support and encourage each other.
Conclusion
Atrial fibrillation is a common heart condition that affects millions of people worldwide. While conventional treatments such as medications and invasive procedures have been used to manage AFib for years, new treatment options are constantly emerging.
Understanding the latest advances in AFib treatment is crucial for patients and caregivers. This guide has summarized AFib, conventional treatments, the latest advances, and factors to consider when choosing a treatment. It has also explored the essential role of patients and caregivers in the AFib treatment process.
Patients and caregivers should work closely with their healthcare team to make informed treatment decisions and actively manage their health. With the right support and resources, individuals with AFib can improve their overall quality of life and potentially reduce the need for invasive procedures or medications.
Why Choose CVG?
At CVG, our cardiologists offer extensive experience caring for patients using state-of-the-art techniques. Their compassion adds so much to your care because our doctors understand how heart issues can affect you physically and take an emotional toll. Trust is the #1 factor in the doctor/patient relationship. You can trust your CVG cardiologist with every aspect of heart care.
Related Conditions:
- Causes And Treatment For Heart Arrhythmia
- Causes And Treatment Of Pulmonary Stenosis
- Expert Insights on Cardiac Catheterization
- Expert Insights on Low Blood Pressure
- Exploring the Latest Advances in Atrial Fibrillation Treatment
- Dangerously high cholesterol?
- Get Your Blood Pressure Test Today!
- Understanding Electrical Cardioversion
- What Are ACE Inhibitors Used For?
- What foods are high in cholesterol?
- What Heart Flutters Can Mean
- What is Heart Failure & How to Treat it?
- What Is The Success Rate Of The Watchman Procedure?
Top Conditions:
- How long can someone live with an enlarged heart?
- Pros and Cons of the Watchman Device
- Risks and Complications of Cardiac Catheterization
- Side Effects Of The Watchman Device
- The Benefits of Cardiac Catheterization
- The Dangers Of High Blood Pressure
- The Dangers Of High Cholesterol
- The Watchman Implant Procedure
- Tips To Lower High Cholesterol
- Understanding Cardiac Catheterization
Call to Schedule an Appointment
Board-certified Doctors
CVG’s twenty board-certified heart doctors will guide you through your healthcare journey with the utmost compassion and individual attention. We aim to provide you with state-of-the-art cardiac care that includes the full spectrum of services, from testing to diagnosis and treatment. The doctor/patient relationship is built on trust. Through our combined efforts, we can conquer any challenge that comes our way.
Invasive therapies may also treat an abnormal heart rhythm, such as electrical cardioversion, which sends electrical impulses through your chest wall and allows normal heart rhythm to restart, or catheter ablation that disconnects the abnormal rhythm’s pathway. Suppose your doctor determines that electrical devices are the best course of action. In that case, you may be given a permanent pacemaker, an implantable cardioverter-defibrillator (ICD), or biventricular (B-V) pacemakers and defibrillators.
How CVG Can Help
CVG offers multiple services that can discover an enlarged heart or conditions that will lead to it. At CVG, we perform stress tests that will observe blood flow and test for various forms of heart disease. There are three types of stress tests that we perform:
- A treadmill test is a test in which you will walk on a treadmill that gets faster and steeper every 3 minutes. This will stress your heart so that our nurse or doctor can determine your heart rate and blood pressure.
- An echo test is performed before and after your treadmill test to determine how well your heart pumps blood.
- A nuclear stress test is a treadmill test that is prefaced by an injection of medicine that shows the flow of blood to your heart.
We also offer cardiac catheterization to diagnose and treat several heart issues. If any of these tests determine a problem, we offer treatment solutions such as atrial fibrillation testing and catheter ablation. Learn more about our services here, or schedule an appointment to talk to our doctors.
Schedule Your Appointment with a CVG Atlanta Area Cardiologist
Expertise, experience, and compassion are the pillars of CVG’s patient-centered cardiac care. Please schedule your appointment with CVG today. Call (770) 962-0399 or 678-582-8586. You may also request an appointment online. If you have an emergency, don’t contact us online; please call 911.
Locations That Treat Atrial Fibrillation













