Electrocardiogram
Most people understand the word electrocardiogram (ECG or EKG). It looks for heart problems by recording your heart’s electrical activity.
Why would your doctor want you to have this test? First, it’s a fast way for the doctor to get insights into your heart’s function and determine arrhythmias (abnormal heart rhythms) or potential coronary disease. An ECG can lead to further tests, like an echocardiogram (heart ultrasound). The benefit of having an ECG performed is that it can help pinpoint or lead to other tests to find the cause behind your symptoms, such as dizziness, weakness, or chest pain.
An ECG is fast and painless. Plus, you may be asked to have associated tests, such as wearing various monitors or performing exercise stress tests so your doctor can observe your heart function.
The ECG helps the doctor discover abnormal heart rhythms and other potential heart problems. The doctor will then arrange a treatment plan or further tests if required.
You can get a quick overview with our CVG Insights: “What is an Electrocardiogram Test?” That article offers an easy point-by-point description of the procedure, and you can read it here for additional information.
CVG’s board-certified doctors and heart team specialists provide the best combination of skill, expertise, and leading-edge technology. You can be assured that your testing will be conducted individually, with the type and duration of monitoring explained to you.
One of the advantages of visiting your CVG heart team is our ten locations. You have enough on your mind without wondering if your doctor is nearby. CVG offers a location near you, so coming to see us is easy. And please be assured that our doctors offer total care, proactively prescribing tests and treatments that benefit you now and helping to ensure your future health.
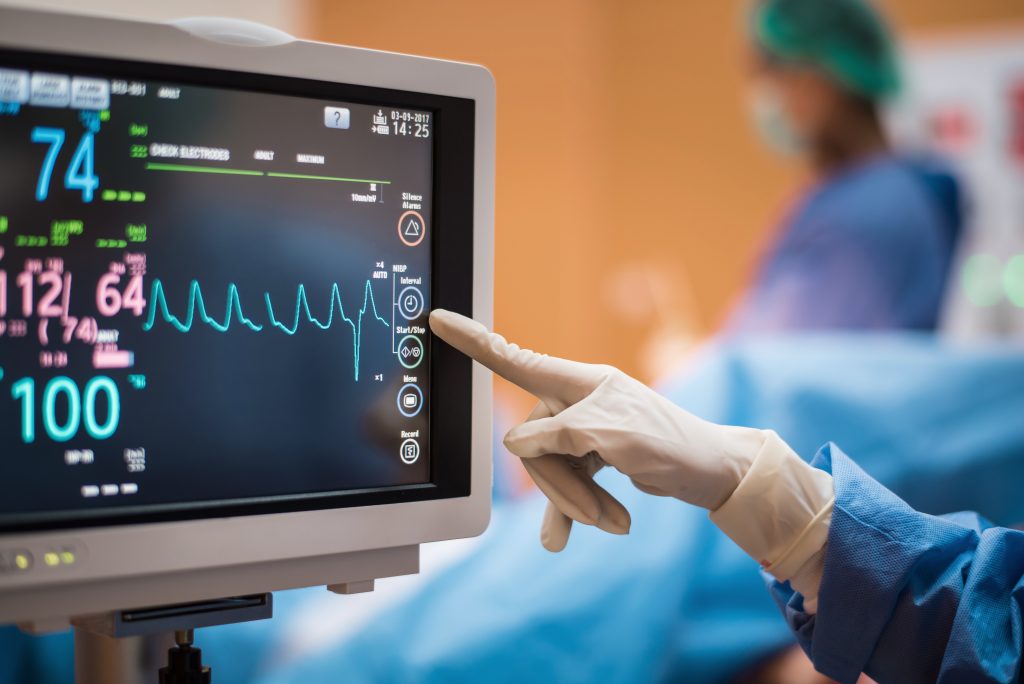
Checking For Signs Of Heart Disease With An Electrocardiogram
An electrocardiogram, called an EKG or ECG, is a quick and painless test that records your heart’s electrical activity to check for signs of heart disease. A technician attaches multiple electrodes to your skin in various body places, tracking electrical impulses.
What Can an EKG Check For?
With an EKG, your doctor can check for multiple potential heart problems. These include irregular heart rhythms, poor blood flow, thickened heart muscle, electrolyte abnormalities, or even heart attacks. Any of these heart problems are risk factors for heart disease.
Heart disease is a catch-all term that includes many types of heart problems, such as arrhythmias, pulmonary hypertension, and, most commonly, coronary artery disease (CAD). With an EKG, you can catch these early before they develop into more serious issues like heart failure.
How Does an EKG Work?
A technician attaches multiple electrodes to the skin on your chest, arms, and legs. During a resting EKG, you’ll lie flat while a computer records your electrical impulses moving through your heart, creating a picture of the activity. A stress test can also be conducted, where the same test is administered to check your heart rate while you exercise. Besides the standard EKG tests, other tests can also be used to test your heart.
A Holter monitor is a portable EKG that monitors the electrical activity of your heart 24/7 over 1 to 2 days. This test may be suggested if your doctor suspects you have an irregular heart rhythm, heart palpitations, or low blood flow. You can go about your daily routine except for showering during this test. You’ll record your activities and any symptoms you notice during this time.
An event monitor is a less intensive test for occasional symptoms. This device has a button you can press whenever you notice symptoms, recording and storing your heart’s electrical activity for a few minutes. Because of the low frequency of this test, you may need to wear the device for weeks or even months.
A loop recorder is a device implanted into your body under the skin of your chest. It has the same functions as an EKG but allows continuous remote monitoring of your heart’s electrical activity. This device searches for irregularities that cause more severe symptoms, such as fainting and heart palpitations.
What Symptoms Should You Get Checked with an EKG?
Suppose you have any of the following symptoms. In that case, it may be time to get an EKG test:
- Chest pain,
- Dizziness or lightheadedness,
- Heart palpitations,
- Shortness of breath,
- Rapid pulse,
- Weakness or fatigue,
- Inability to exercise.
If your family has a history of heart disease, your doctor may suggest an electrocardiogram even if you aren’t displaying any symptoms.
Risks Of An EKG
There are little to no risks involved with EKG testing. Some people with skin sensitivity can experience a rash where the electrodes are placed; however, this usually goes away independently. Patients who undergo the stress test may be at risk of a heart attack, although this is related to the exercise and not the EKG itself.
An EKG only monitors the electrical activity of your heart; it does not emit any electricity. This means the device is completely safe, even during pregnancy.
How To Prepare for an EKG
While getting ready for your EKG, there are a few things to consider:
- Remove any jewelry.
- Shave hair in areas where the electrodes will be placed.
- Avoid drinking cold water directly before the test (this can cause changes in electrical patterns).
- Do not participate in any exercise or other activity that will increase your heart rate before the test.
- Keep the room at a moderate temperature to avoid shivering (movement will affect the accuracy of the results).
Results Of An EKG
Your EKG results can sometimes be available the same day as your test or by the next appointment. The results of an EKG will give your doctor more details about the following issues:
- Heart rate: Heart rate can typically be measured by checking your pulse. An EKG is helpful if your pulse is irregular, too fast, too slow, or at odd moments. In these instances, your pulse will be difficult to determine regularly. An EKG can help determine an abnormally fast heart rate (tachycardia) or an unusually slow heart rate (bradycardia).
- Heart rhythm: An EKG can decide if you have an irregular heartbeat (arrhythmias). Arrhythmias can occur if parts of the heart’s electrical system aren’t working properly.
- Heart attack: An EKG can show evidence of previous heart attacks or a current one. It helps to give detailed results on which part of the heart has been damaged and the extent of the damage.
- Blood and oxygen supply: An EKG done while experiencing symptoms will help your doctor determine if chest pain is caused by reduced blood flow to the heart.
- Heart structure: An EKG can provide doctors with more information about whether you have an enlarged heart, heart defects, or other heart issues.
How CVG Can Help?
CVG offers electrocardiograms to assess your risks of heart disease. We provide various EKGs so that we can determine how your heart is functioning and what steps you will need to take to prevent further problems. If these tests determine a problem, we offer treatment solutions to help against heart disease.
Learn more about our services here, or schedule an appointment to talk to our doctors.
Frequently Asked Questions
An ECG is a medical test that records the electrical activity of the heart over a period of time, providing information about heart rate, rhythm, and potential abnormalities.
- ECGs are used to diagnose various heart conditions, including arrhythmias, heart attacks, and other cardiac issues. They are also utilized to monitor heart health in patients with existing heart conditions.
- During an ECG, electrodes are placed on the skin of the chest, arms, and legs to detect electrical signals from the heart. The procedure is non-invasive, painless, and typically takes about 5 to 10 minutes.
Yes, there are several types of ECGs, including:
- Resting ECG: Performed while the patient is at rest.
- Stress ECG: Conducted during physical exertion to assess how the heart responds to stress.
- Holter Monitoring: A portable device worn for 24–48 hours to monitor heart activity over an extended period.
An ECG can identify various heart-related issues, such as:
- Irregular heart rhythms (arrhythmias)
- Heart attacks (both previous and current)
- Enlarged heart chambers
- Electrolyte imbalances
Generally, no special preparation is required. However, it’s advisable to avoid applying lotions or oils on the skin before the test, as they can interfere with electrode adhesion. Wearing comfortable clothing that allows easy access to the chest area is also recommended.
ECGs are safe and non-invasive procedures with no significant risks. Some individuals may experience minor skin irritation from the adhesive electrodes, but this is uncommon.
Our healthcare provider analyzes the ECG tracing to assess the heart’s electrical activity. Deviations from normal patterns can indicate various heart conditions, which the provider will discuss with the patient.
While an ECG is a valuable tool for diagnosing many heart conditions, it may not detect all issues, especially if they are intermittent. Additional tests, such as echocardiograms or stress tests, may be necessary for a comprehensive evaluation.
An ECG is recommended if you experience symptoms like chest pain, shortness of breath, dizziness, or palpitations. It may also be advised if you have a family history of heart disease or as part of a routine check-up in certain situations.

